A multidisciplinary team with Master of Applied Bioengineering students at its core is building WiseFind AI. The AI-based tool will make electronic medical records easier to use and provide the students an unparalleled opportunity for real-world impact.
A patient arrives in the emergency room after a car accident. Clinicians begin their assessment. They evaluate the patient’s motor function and other indicators for what is known as the Glasgow Coma Scale. They evaluate the patient’s body parts for signs of trauma for an Injury Severity Score. Vitals, CT scans, and abundant notes are taken.
A host of data is recorded on various electronic medical record platforms. The data is often collected very quickly, and things can get messy. It’s all crucial to diagnosis, treatment, and long-term outcomes of traumatic brain injuries and spinal injuries.
A quartet of students from Bioengineering’s Master of Applied Bioengineering (MAB) program have teamed with a pair of professors from UW’s School of Medicine to tame these unruly records. Together, they are building an AI tool that will help practitioners extract specific clinical information from medical records, minimize missed relevant data, and make the records easier to use in future research programs and clinical applications.
The MAB students include Dr. Aruna Souri (already a neurologist herself), June Lee and Mary Nguyen (both experienced software engineers), and Benjamin Han (an alumnus of UW’s Bioengineering undergraduate program).
“The students in our program come from a variety of backgrounds and are already immensely skilled, but looking to grow in new areas. Their professional colleagues truly commit to mentoring students and help them build their relationship to content and address real clinical needs,” said Professor Rupak Rajachar, who oversees the Master of Applied Bioengineering program.
They call their solution to those real clinical needs “WiseFind AI.”
“There’s a dark side to medicine. Details get lost in the effort to keep up. We spend hours in electronic medical records trying to document how we diagnosed the patient and why we chose a treatment option versus others,” said Dr. Diana Wiseman, a clinical professor of neurological surgery at UW Medicine and Harborview Medical Center and a former Navy neurosurgeon. Her colleague on the team is Dr. Christopher Lewis, an assistant professor in rehabilitation medicine at UW Medicine. He is an expert in electronic medical records and the department’s first chief clinical information officer.
“The pace that you see in trauma service on shows like The Pitt is relentless. It’s real.”
Thinking Like a Doctor
Having worked together for only a matter of months, the team has already earned a $25,000 grant from the Institute of Translational Health Sciences, which is a partnership among the University of Washington, Fred Hutchinson Cancer Center, and Seattle Children’s Hospital. Wiseman and Lewis have also applied for funding from UW’s CoMotion and are receiving training through the National Science Foundation’s I-CORPS program to expand WiseFind AI.
“We’re teaching a Large Language Model from Google that focuses on the medical domain, called MedGemma, to think like a doctor. We want to incorporate clinical neurotrauma texts, give them priority, and identify important elements,” said Souri, who completed her residency at HCA HealthONE Swedish Medical Center in Denver before joining the MAB program.

In the team’s estimation, clinical use of artificial intelligence requires two things: The AI needs to be able to make sense of the electronic health records of real patients, even though they are often in free-written, unstructured text, and it needs to be able to collate and characterize injuries using standard injury scales in a transparent fashion to assure quality. It will also fill gaps in those records in ways that are transparent and explainable to the clinicians who would use the tool.
“For the doctors, it’s a time problem, a human capital problem. We want them treating patients, not filling out records. We don’t want them mindlessly transcribing information in different spots and different formats. That work seems like a great use for AI,” Lewis said.
“No matter what we’ve built to make that process easier in electronic medical records, it just never has been easy enough. It’s a scattered hodgepodge that’s very hard to make your way through. It’s death by a thousand clicks,” Wiseman continued.
Foundational Models and Agents
Any tool of this sort will require a foundational AI model for brain and spinal cord injury. Large Language Model-based platforms like ChatGPT or Claude allow developers to build applications on top of their models and leverage their existing AIs. But these platforms are not well-enough trained on the specialized vocabulary that fills medical records and charts. They don’t speak the language.
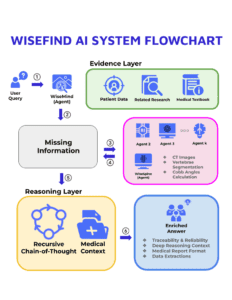
To address that challenge, the team is building what is known as a retrieval-augmented generation framework, or RAG. The RAG will allow existing AIs to access additional databases and other information focused on brain and spinal cord data. The team will then be able to use existing AIs without retraining them entirely. The RAG will also significantly reduce errors and decrease the likelihood of the AI making up false information.
“Ask ChatGPT now, and it won’t understand GCS [the Glasgow Coma Scale well enough to work for doctors.] We need to build on that knowledge foundation with traceable sources that we can trust,” said June Lee, who spent six years as an AI developer at a medtech company before entering the MAB program.
Lee plans to build AI agents – automated assistants that can be given a task, then research the problem and take action to address it. These will support users as they address and study brain and spine injuries. (Find more about one of WiseFind AI’s agents in the sidebar “A New Angle on AI.”)
Nguyen, meanwhile, will focus on the user-interface and backend functionality of WiseFind AI and future AI agents, enabling users to interact directly with the AI model alongside tools for storing and retrieving medical context. Nguyen modernized electronic criminal medical records within the Legal Information Network Exchange, improving accessibility and usability for the Judicial & Safety Department in Pierce County, Washington, before starting the MAB program.
“I plan to apply my full-stack engineering experience so that WiseFind AI can be integrated smoothly into clinicians’ workflows. My focus is on building the interfaces that clinicians interact with in real time, enabling them to see the evidence, sources, and citations behind the model’s responses,” Nguyen said.
Han is standing up a demo version of the RAG-enhanced Large Language Model and its interface on a server, optimizing backend performance so an alpha version of the system can be tested.
For example, “I am currently finding ways to both reduce latency for a single user and allow multiple users to easily access the WiseFind AI program on different devices” said Han, who worked at the skincare technology company Bio-Theraputics automating customer service data-related tasks before returning for his MAB.
The team recently received approval from UW’s Institutional Review Board and is beginning to train the AI with real-world patient data.
One of WiseFind AI’s first tasks will be to train on a small segment of brain and spine injury characterizations that are crucial to define injury patterns, or combinations of injuries that indicate the cause of those injuries. With that complete, they will assess how well the program can categorize these injuries based on those patterns and fill in the gaps clinicians currently see in traumatic injury registries. These registries are an important tool for tracking the quality of patient care. They are also used to support research and community- and national-scale public health efforts.
The AI model can assist the clinical team by filling in those gaps from the data already present in their notes. This process will save teams time because they won’t have to fill in these data elements manually. The results will also help support future quality improvement projects and research on brain and spinal cord injury with the ultimate aim of improving outcomes for patients.
“This team – with their many backgrounds and skillsets – are working on concrete applications with meaningful impact together,” Rajachar said. “This reflects our shared vision of the MAB program, and it illustrates why the program is so valuable to everyone involved.”
A Different Angle on AI
In addition to text-based patient data, the team is also developing an imaging-focused AI agent called WiseSpine as part of WiseFind AI.
WiseSpine is designed to analyze spinal imaging data and assist clinicians in understanding the severity and mechanisms of spinal injuries. The system will automatically segment vertebrae, estimate clinical measurements such as the Cobb angle, and predict injury classifications, such as the AO Spine classification.
Beyond image analysis, the team plans to integrate a spine physical simulation model that reconstructs spinal biomechanics. This simulation framework will allow the system to infer possible injury mechanisms and explore the potential outcomes of different surgical strategies.
The goal is to move beyond statistical measurements and provide clinicians with an AI-assisted biomechanical understanding of spinal injuries.



