BE A WORLD OF GOOD
What do at-home disease test kits, neuroscience and the fit of artificial limbs have in common? Not much, it would seem, beyond each being part of UW Bioengineering’s wildly diverse fields of research. But a shared thread connects these projects and others in the department: the researchers’ dedication to serving the public good and improving health.
The people who benefit from UW Bioengineering research range from Seattleites to remote villagers in all corners of the world – and from amputees to schoolchildren to anyone who’s ever wondered if they have the flu. Now, three researchers talk about the motivations for their work and the impact it stands to make.
If you can’t bring the person to the lab, bring the lab to the person
In one way, Paul Yager grew up in the future, immersed in the science fiction of Jules Verne, Ray Bradbury and Star Trek, all of which sparked his passion for science. In another way, he was very much in reality as he sat with his ill mother for long hours in New York City public health clinics. “I remember those times being long and unpleasant and scary experiences, and I think that may have been a deep motivation for me at one level,” Yager says. “It wasn’t a lot of fun being someone who had to wait a long time to see a doctor, whether it was you or a parent.”

His associations with colleagues at PATH and funding he received from the Gates Foundation in 2005 ignited his interest in global health. Road trips with the Gates Foundation to a township in South Africa, shrimp farms in southern Thailand and areas of Tanzania showed him the specific problems and limitations communities in the developing world often face. “I think seeing what actually went on with my own two eyes was a big motivator for me,” he says.
With roads in the developing world often impassable, and no access to sophisticated lab equipment, Yager saw a great need to bring medical testing to the patient. “What’s annoying and time-consuming in the U.S. can be life-endangering in the developing world, either because you can’t do it that way, or it would take so long the patient could be dead by the time you get an answer,” Yager told the audience at a TEDx talk in Seattle Nov. 22.
Yager’s research team, including Barry Lutz, assistant professor, and numerous collaborators, focuses on simplicity: the tests they are developing need no power, special equipment or running water. They could be stored in a pouch up to a year at room temperature. “Simplicity and low-cost are critical, and that it’s rapid and robust – meaning I could store it in the glove compartment of my car or in a home in Guali,” Yager says.
 To use the test, you take a nasal swab sample, swirl the swab in the test box for 10 seconds, close the lid and wait 20-50 minutes, depending on the type of test. Results appear in a window, and the goal is that you could then take a picture with your cell phone, which could quickly analyze the results and send them to a doctor for review and treatment instructions, effectively extending the doctor-patient relationship back to the home or wherever the patient is.
To use the test, you take a nasal swab sample, swirl the swab in the test box for 10 seconds, close the lid and wait 20-50 minutes, depending on the type of test. Results appear in a window, and the goal is that you could then take a picture with your cell phone, which could quickly analyze the results and send them to a doctor for review and treatment instructions, effectively extending the doctor-patient relationship back to the home or wherever the patient is.
Programming in paper: Read about how the test works
The tests could diagnose pathogens such as flu, MRSA, HIV, malaria or Ebola. Yager suggests the test could be used to screen for Ebola during an outbreak, allowing people to test at home and minimizing potential exposures. Prompt testing for sexually transmitted diseases, such as HIV, would allow an individual to get post-exposure prophylactics and avoid a life on anti-retroviral drugs. “This is a huge significance in the developing world,” Yager points out. And, it’s possible farmers could check the health of their animals or crops.
“The ability to move the test right to the patient is the thing I hear over and over as being the big success of this if it works,” Yager says. “We can save time, money and suffering if we can do testing at home instead of bringing people to the hospital.”
Yager described his passion this way: “We do it partially because we love the technology, we’re engineers. We also do it because we think that distribution is fair. It’s the right thing to do for people. It’s something that we need to do to help the world. And finally, it makes us all healthier and safer.”
Brain awareness starts kids on path to science literacy
If there is a teacher gene, neuroscientist Eric Chudler must have inherited it. Both his parents were teachers. So when faced with explaining neuroscience to a group of 3-5-year-olds at his daughter’s preschool career day, Chudler pulled out a bag of potato chips. He delighted in getting them to explore their senses and how their brains worked by imagining the crunch and the taste. As his daughter grew, he continued to visit her classrooms and give presentations.

By the mid-90s, Internet use was on the rise. “I thought, ‘Wouldn’t it be a good idea if this Internet thing could be used for education?’ I could expand what I’m doing to reach people around the world.” In 1997, with funding from an NIH Science Education Partnership Award, Chudler created the website Neuroscience for Kids, a site to help teachers and kids learn about the nervous system. The grant helped him collaborate with teachers to make sure the materials were grade-appropriate. Although funding ran out in the early 2000s, he still updates the site occasionally, and writes a monthly newsletter that goes to 10,000 subscribers.
If you Google the term “neuroscience,” Chudler’s Neuroscience for Kids page typically appears in the top five results. Sections of site have been translated into 13 languages.
Also in the late 90s, Chudler launched UW’s Brain Awareness Week, supported in part by the Society for Neuroscience. What began as a grassroots effort now brings 700 local elementary to high school-age students to the UW campus annually to learn about the university and its neuroscience research.
Today, Chudler directs Sowing the Seeds of Neuroscience, also known as Neuroseeds, a partnership among neuroscience researchers, teachers and students. The project supports research and outreach, and is funded with a Blueprint for Neuroscience Research grant through the NIH’s National Institute on Drug Abuse. Chudler conducts research about the neuroactive properties of plants and herbs, the sources of many medicines. “Western science knows only a fraction about what other cultures use around the world,” Chudler says. His lab work with invertebrates aims to reveal whether such plants have true neuroactive properties.
Chudler and his team convert the basic knowledge gained in the lab into curricular materials that students and teachers can use in middle schools. Neuroseeds hosts annual summer teacher workshops that train them how to use the materials. After completing their professional development, teachers can check out kits with everything they need to do experiments in the classroom. In return, teachers and kids evaluate the kits and how much they learned about neuroscience. “I’m especially interested in changes in attitudes about how students view science – whether science is something they would pursue in the future and something they find valuable,” Chudler says. “Do they see the value of science to society and does that change after they use the Neuroseeds materials?” He hopes to further explore this idea with a group of students who are not already enrolled in science classes.
The Neuroseeds grant also includes a one-week camp for middle school students called Bloomin’ Brains Summer Camp. Over the past two years, the camp has brought about 50 students to campus to conduct hands-on experiments, tour neuroscience labs and the medicinal garden, learn about an herbal first aid kit and play games based on neuroscience concepts.
Other outreach includes hosting school group visits to the Center for Sensorimotor Neural Engineering to teach about activities and research. Chudler or his students also occasionally go out to schools to give presentations. Eight years ago, Chudler collaborated with UWTV on a show called BrainWorks. Nominated for a Northwest Emmy Award, it is still UWTV’s second most popular show. He’s also traveled to India four times since 2011 to do outreach through the Science for Monks program. “It’s very rewarding but difficult,” he says. (Read about his most recent experience.)
Chudler cites two main reasons for his dedication to outreach. He wants to raise science literacy and to show the public how their tax dollars are being used. “I suppose it’s a bit self-serving for science,” he says. “It’s my belief that a knowledgeable public will see what science does in a more favorable light, so when they see their tax dollars funding science, they can see the rewards that science brings.”
Chudler says most everyone will be affected by neurological disease, whether it’s a traumatic brain injury, mental illness or neurological illness in a friend or family member, or important person in the news. “Perhaps by making the public more aware of the issues, they can make better decisions for themselves or people they know,” he says. “Or at least understand how to evaluate scientific claims being made in the news. Science issues might also be on a ballot, or people may sit on a jury that requires critical thinking about scientific evidence. These things are all going to affect the social fabric of society.”
“Smart” prostheses fit the need for amputees
Joan Sanders’ research makes a direct impact on day-to-day life – in fact, hour-to-hour life –for people who have had a limb amputated. Dr. Sanders’ research is focused on optimizing the fit between the prosthetic socket and the user’s residual limb, reducing or eliminating pain and improving function.

“Prosthetics is an interesting field because there’s a lot of very technically sophisticated stuff out there – robotics almost articulated ankles and feet, and from an engineering perspective they do wonderful things,” Sanders says. “But if the prosthesis doesn’t fit right, it doesn’t help. We are really concerned with filling that void.”
Technologies exist that can adjust the size of the socket over time by pressing a button or activating a control. But, Sanders says, they don’t come with information about how to use them or when to adjust the socket larger or smaller. To fill this need, Sanders and her team have developed various real-time sensing devices, most of which are portable. Their instruments provide real-time information on recent volume changes in the limb and suggest how to adjust the socket to enhance the fit.
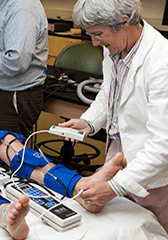
Prosthetics is a relatively small field. “We have a big impact with so many years of experience doing what we’ve been doing. Our results are typically well-received and used,” Sanders says. “Seeing the impact of what you’re doing right away in the clinic is very satisfying to my staff and me.”
Sanders’ research is tightly linked to the UW Department of Rehabilitation Medicine, the highest ranked hospital-based rehab program in the country. The research fits perfectly into the department’s clinical mission, providing instrumentation and measurement in prosthetic biomechanics. “The collaborations with Rehabilitation Medicine faculty are key our success,” Sanders notes.
“We’re always seeking feedback from amputees,” Sanders says. “We want to hear about their issues and needs. And what it’s going to take for us to have a greater presence in their treatment environment. The field of prosthetics is very opportunistic and we look forward to continuing to contribute to improve the quality of life of people with limb loss.”





