Michael L. and Myrna Darland Endowed Chair in Technology Commercialization Professor of Bioengineering and Chemical Engineering
ratner@uw.edu
Phone: (206) 685-1005
Office: Foege N330J
Buddy D. Ratner
Medical devices and implants are engineered from specially designed materials, often referred to as biomaterials. Millions of devices and implants are used clinically in applications as diverse as blood vessel replacements, catheters, contact lenses, hip joints, ventricular assist devices and artificial kidneys. The biocompatibility of these prostheses is dictated by their surface properties and by the local mechanical environment they induce. In my research program, biomaterials are engineered to control biological interactions. We seek to redefine “biocompatibility” to mean a new level of compatibility with the body — a true biointegration with living tissues and organs. By synthesizing new biomaterials that accurately direct biological response, or are “stealth” so the body does not see them, we believe we can invent a new future for biomaterials and implanted medical devices.
biomaterials
surface modification
blood compatibility
biocompatibility
protein adsorption
membranes
vascular grafts
stents
catheters
skin healing
hydrogels
polyurethanes
plasma-deposited thin films
We engineer new biomaterial surfaces using a wide range of technologies. For example, radio-frequency plasma deposition (a method borrowed from microelectronics) can readily place interesting thin films on existing medical device surfaces. These films can be used in the precision immobilization of key signaling molecules. We also synthesize new polymers that can be biostable, environmentally responsive, biodegradable and/or porous (i.e., scaffolds). The new surfaces and materials made in our laboratory are studied in contact with proteins, blood, living cells and tissues (in vivo and in vitro).
Recently, there has been considerable interest in tissue engineering in my laboratory. Tissue engineering exploits all the above principles in the context of tissue and organ reconstruction and regeneration. Specific tissue engineering projects in the Ratner lab have aimed toward heart muscle, esophagus, bone, cartilage, bladder, vagina and cornea. Another new project seeks to model cancer tumor microenvironments using tissue engineering ideas.
Biomaterials/biocompatibility projects ongoing in my laboratory include:
- drug delivery devices
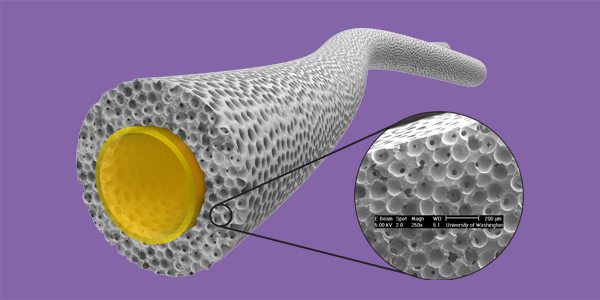
- porous scaffolds
- tissue engineering
- angiogenesis
- healing in soft tissue
- bioelectrode performance
- bioattachment
- biorecognition
- polyurethanes
- hydrogels
- biodegradable polymers
- non-fouling surfaces
- blood-contacting materials
- bacterial biofilms/infection
Biomaterial surfaces are the only part of a biomaterial or medical device that is seen by the body. Surfaces present unique analytical problems because of the small mass of material involved (a billionth of a gram of matter per square centimeter is typical). Special instruments are required to study surfaces, and we adapt methods developed in the physics and microelectronics communities to problems in biology and medicine. We use electron spectroscopy for chemical analysis (ESCA), secondary ion mass spectrometry (SIMS), infrared spectroscopy, scanning probe microscopies, surface plasmon resonance and sum frequency generation to observe surface structure and biological interactions.
In 2016, we launched the Center for Kidney Dialysis (CDI). CDI aims to address many of problems in kidney dialysis that shorten the lives of patients including blood compatibility, fibrosis, restenosis, bacterial infection, membrane limitations, etc. I serve as co-director of CDI along with Professor Jonathan Himmelfarb (MD nephrologist).
BS, Chemistry, Brooklyn College, 1967
2016 Kammermeyer Lecturer, University of Iowa
2015 Distinguished Service Award, ACS Division of Polymer Chemistry
2015 Langmuir Lecture, American Chemical Society (COLL Division)
2015 Most Cited Paper Award, Annals of Biomedical Engineering
2014 Fellow, Polymer Division of American Chemical Society
2014 University of Washington School of Medicine 2014 Lifetime Innovator and Inventor Award
2011-2012 AVS Biointerphases Lectureship
2010-2012 UW Entrepreneurial Faculty Fellow
2012 George Winter Award, European Society for Biomaterials
2012 Honorary Professor of Sichuan University
2012 Journal of Materials Science-Materials in Medicine “Best Paper Published in 2011”
2012 Fellow, Tissue Engineering and Regenerative Medicine International Society (FTERM)
2011 Pierre Galletti Award of the American Institute of Medical & Biological Engineering
2011 Fellow, American Chemical Society
2010 McGowan Distinguished Lecturer, University of Pittsburgh
2010 Annual Faculty Lecturer, University of Washington
2009 Chandra P. Sharma Award, Society for Biomaterials & Artificial Organs (India)
2009 Acta Biomaterialia Gold Medal Award
2008 BMES Pritzker Distinguished Lecturer Award
2008 J. Edward Berk Lecture Medal
2008 Listed in AIChE’s “One Hundred Chemical Engineers of the Modern Era”
2008 Frontiers of Science Award, Society of Cosmetic Chemists
2008 Kewaunee Lecturer, Duke University
2007 Bayer Lectureship, University of Akron
2006 C. William Hall Award, Society for Biomaterials
2004 Founders Award, Society for Biomaterials
2004 Distinguished Lecturer, University of Utah
2002 Elected to the National Academy of Engineering of the United States of America
2002 Medard W. Welch Award, American Vacuum Society
2002 Chair, Roundtable on Biomedical Engineering Materials and Applications (BEMA)
2000 Science In Medicine Lecturer, University of Washington
2000 Joe Smith Distinguished Lecturer, University of California, Davis
2004-2005 Robert F. Rushmer Professor of Bioengineering, University of Washington
2001-2004 Washington Research Foundation Endowed Professor of Bioengineering
1999 American Vacuum Society Distinguished Lecturer
1998 C.M.A. Stine Award for Materials Science, AIChE
1996 Van Ness Lecturer, Rensselear Polytechnic Institute
1995 Chair, Gordon Research Conference on Biocompatibility & Biomaterials, July 23-28
1993 Founding Fellow of the American Institute of Medical and Biological Engineering (AIMBE)
1993 Fellow, American Vacuum Society
1993 Fellow, Society for Biomaterials
1991 Perkin Elmer Physical Electronics Award for Excellence in Surface Science
1990 Burlington Resources Foundation Faculty Achievement Award for Outstanding Research
1988 Clemson Award for Contributions to the Literature
BIOEN 492/592: Surface Analysis
BIOEN 490: Biomaterials
BIOEN 504: Introduction to Technology Commercialization
BIOEN 505: Biomedical Entrepreneurship
BIOEN 511: Biomaterials Seminar
1. “An Innovation Ecosystem: The Center for Dialysis Innovation (CDI)” Buddy Ratner and Jonathan Himmelfarb, Journal of the American Society For Nephrology, 35, 1119-1122, 2024
2. “Vascular Grafts: Technology Success/Technology Failure,” Buddy Ratner, Biomedical Engineering Frontiers, 4: Article 0003. https://doi.org/10.34133/ bmef.0003, 2023
3. “Dialysate Regeneration with Urea Selective Membrane Coupled to Photoelectrochemical Oxidation System” Guozheng Shao, Hao Tang, Shen Ren, Sharon A. Creason, Dayong Gao, Buddy Ratner, and Bruce J. Hinds, Advanced Materials Interfaces, 9(13), 2102308, 2022
4. “Polyurethane-based, mechanically-matched angiogenic, precision-porous long-lasting elastomers for pro-healing vascular grafts and in situ vascular engineering applications”, Le Zhen, Sharon Creason, Felix Simonovsky, Jessica M. Snyder, Sarah A. Proffitt, Marvin M. Mecwan, Brian W. Johnson, Jonathan Himmelfarb, Buddy Ratner, Biomaterials, 279 121174, 2021
5. “Biocompatibility Evolves: Phenomenology to Toxicology to Regeneration,” Lars Crawford, Meghan J. Wyatt, James D. Bryers, Buddy D. Ratner, Advanced Healthcare Materials, 2002153, 2021
6.”Photo-reactive carboxybetaine copolymers impart biocompatibility and inhibit plasticizer leaching on polyvinyl chloride” Xiaojie Lin, Kan Wu, Qiong Zhou, Priyesh Jain, Mary O’Kelly Boit, Bowen Li, Hsiang-Chieh Hung, Sharon A. Creason, Jonathan Himmelfarb*, Buddy D. Ratner, Shaoyi Jiang, ACS Applied Materials & Interfaces, 12, (37) 41026–41037 2020
7. “Biomaterials: Been There, Done That, and Evolving into the Future,” B.D. Ratner, Annual Reviews of Biomedical Engineering, 21, 171–91 2019
8. “A Pore Way to Heal and Regenerate: 21st Century Thinking on Biocompatibility” B. D. Ratner, Regenerative Biomaterials, 3 (2): 107-110, 2016
9. “Blood Compatibility Assessment of Polymers used in Drug Eluting Stent Coatings,” Luisa Mayorga Szott, Colleen A. Irvin, Mikael Trollsas, Syed Hossainy, Buddy D. Ratner, Biointerphases, 11. 029806, 2016
10. “Porous implants modulate healing and induce shifts in local macrophage polarization in the foreign body reaction,” E.M. Sussman, M.C. Halpin, J. Muster, R.T. Moon, B.D. Ratner, Annals of Biomedical Engineering, 42(7):1508-16, 2014.
In the News
Sessions hosted in honor of Ratner at Society for Biomaterials meeting
2026-03-17T07:54:17-07:00March 17th, 2026|
Ratner earns NIH tech transfer grant to improve dialysis for patients
2025-10-17T05:46:56-07:00October 17th, 2025|
2023 Hoffman Lecture – Buddy Ratner
2026-03-17T08:02:38-07:00September 28th, 2023|
Two BioE undergrads receive Population Health Recognition Awards
2026-03-17T08:23:21-07:00June 2nd, 2022|
Monocytes contribute to a pro-healing response in 40 µm diameter uniform-pore, precision-templated scaffolds
2022-04-19T10:51:58-07:00April 19th, 2022|
Precision-engineered porous, flexible grafts promote healing, reduce scarring
2026-03-16T07:26:07-07:00December 15th, 2021|